
Types Of Breast Cancer: What You Need To Know
Breast tissue contains a complex network of ducts, lobules, and connective structures, which explains why...
Read MoreAbnormal Pap test results often begin the medical journey that answers the question of how to test for cervical cancer in a structured clinical pathway. These findings can appear before any noticeable symptoms develop, making early evaluation a central step in cervical health care.
Human papillomavirus testing and Pap screening often detect cellular changes that require closer examination through follow-up procedures. Some individuals also enter testing after symptoms such as irregular vaginal bleeding or discomfort during intercourse appear.
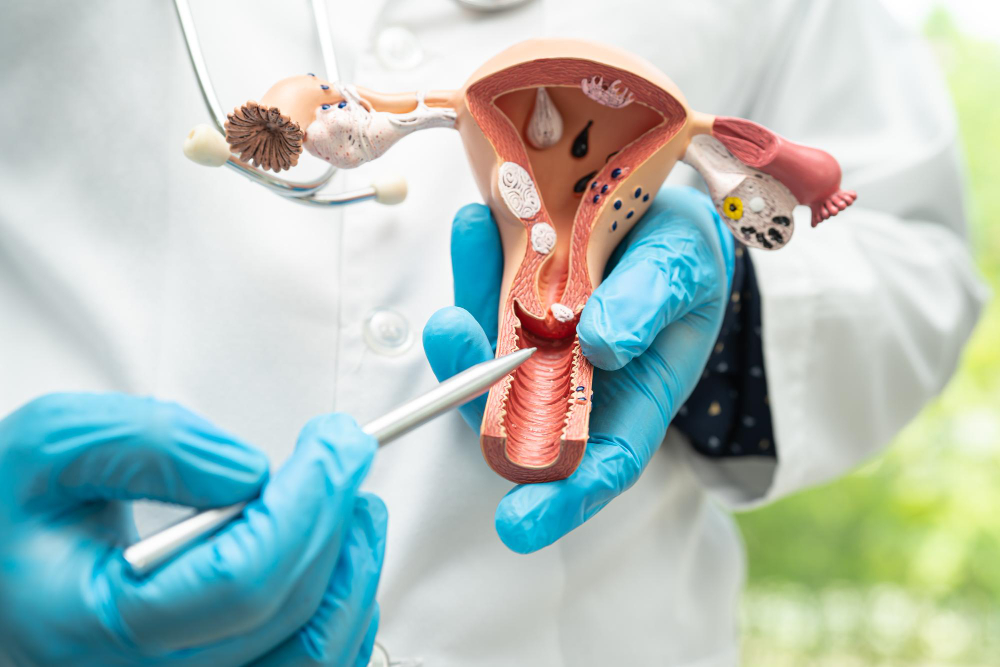
A stepwise diagnostic process helps distinguish between harmless cellular changes, precancerous conditions, and invasive disease through carefully selected examinations and laboratory analysis.
Cervical cancer often develops gradually through cellular changes in the cervix that may remain silent for years. Screening tests aim to identify these changes before they progress further. The cervix can undergo precancerous transformations caused primarily by persistent infection with high-risk human papillomavirus types.
Screening begins long before symptoms because early cellular changes rarely cause pain or visible signs. Many individuals feel completely well while abnormal cells develop. Regular cervical screening allows healthcare professionals to identify microscopic changes that cannot be detected through physical sensation alone.
When screening detects irregularities, clinicians move toward diagnostic testing. This step differentiates temporary infections or minor changes from lesions that may require medical attention. The process is structured to avoid unnecessary intervention while identifying conditions that need closer examination.
The Pap test remains one of the most widely used screening methods in gynecological care. During this test, cells from the cervix are gently collected and examined under a microscope. The aim is to identify abnormal cellular patterns that could indicate precancerous changes.
HPV testing evaluates the presence of viral strains known to increase the risk of cervical cancer. High-risk HPV types are responsible for the majority of cervical cancer cases worldwide. When used together, Pap and HPV tests offer a clearer picture of cervical health than either test alone.
These screening tools do not confirm cancer. Instead, they signal the need for further investigation when irregular results appear. A normal result often leads to routine follow-up screening at recommended intervals, while an abnormal result leads to additional evaluation steps.
An abnormal Pap or HPV test result does not automatically indicate cancer. Many abnormalities resolve naturally, particularly when caused by temporary viral infections. However, persistent abnormalities require careful evaluation.
Healthcare professionals assess current results alongside previous screening history. This combined review helps estimate the likelihood of progression toward cervical cancer. The decision for follow-up testing depends on this risk assessment rather than a single result.
In some cases, repeat testing may be scheduled. In others, direct examination of cervical tissue becomes necessary. The goal is to distinguish harmless cellular changes from those that show signs of progression.
Colposcopy is often the next step after abnormal screening results. This procedure allows a detailed visual examination of the cervix using a magnifying instrument called a colposcope.
During the examination, the cervix is gently exposed using a speculum. A mild acetic acid solution is applied to highlight abnormal areas. These areas may appear white or change texture when viewed under magnification.
If irregular tissue is identified, a biopsy is taken. This small tissue sample is then examined in a laboratory to determine the nature of the cellular changes. Colposcopy itself does not diagnose cancer but directs where tissue sampling should occur.
The procedure is typically performed in an outpatient setting and may cause mild discomfort similar to a routine pelvic examination.
Biopsy results play a central role in confirming cervical precancer or cancer. Several biopsy methods may be used depending on the location and appearance of abnormal tissue.
A colposcopic biopsy removes a small section of visible abnormal tissue from the cervix. The sample is collected using a specialized instrument and sent for laboratory evaluation. Mild cramping or slight bleeding may occur after the procedure.
When abnormal areas are not clearly visible or extend into the cervical canal, an endocervical curettage may be performed. A small brush or curette is used to gently collect tissue from the cervical canal. This area cannot always be fully seen during colposcopy, making sampling important in certain cases.
A cone biopsy removes a cone-shaped section of cervical tissue that includes both surface and deeper layers. This method allows examination of the transformation zone, where precancerous changes often begin.
Two main techniques are used. Loop electrosurgical excision uses a thin heated wire loop to remove tissue in an outpatient setting. Cold knife conization uses a surgical scalpel in a hospital environment under anesthesia.
Cone biopsy can diagnose and sometimes remove abnormal tissue entirely. In some cases, it becomes the only treatment needed for early lesions.
If biopsy results confirm cancer, further tests may be used to determine the extent of disease spread. These tests help guide the next phase of medical decision-making.
Imaging studies often include CT scans, MRI scans, and PET/CT scans. Each method offers different insights into tissue structure and potential spread to lymph nodes or distant organs. Chest X-rays may also be used to examine lung involvement.
In certain situations, cystoscopy and proctoscopy are performed. Cystoscopy examines the bladder using a thin camera inserted through the urethra. Proctoscopy evaluates the rectum for signs of cancer spread. These procedures are typically reserved for more advanced cases.
An examination under anesthesia may also be performed to allow a thorough pelvic evaluation without discomfort.
Staging describes how far cervical cancer has progressed. This classification guides treatment planning and helps determine the extent of disease.
Stage 0 refers to precancerous changes confined to the cervical lining. Stage I indicates cancer limited to the cervix. Stage II shows spread beyond the cervix into nearby tissues. Stage III involves more extensive pelvic spread and possible kidney function impact. Stage IV represents distant spread to organs such as the bladder, rectum, liver, or lungs.
Accurate staging depends on biopsy results, imaging studies, and physical examination findings. Each stage reflects a different level of tissue involvement and guides clinical decisions.
Treatment options depend on stage, overall health, and tissue findings. Early-stage cervical cancer may be treated with surgical removal of affected tissue. In some cases, procedures such as cone biopsy or loop excision remove abnormal areas completely.
Advanced cases may require hysterectomy for cervical cancer, where the uterus is surgically removed. This procedure is considered when cancer extends beyond superficial layers or when recurrence risk is high.
Radiation therapy and chemotherapy may also be used when cancer spreads beyond the cervix. These treatments target remaining cancer cells and reduce further progression.
Each treatment plan is individualized based on diagnostic findings and overall health considerations.
After treatment or abnormal findings, long-term monitoring becomes part of routine care. Follow-up visits may include repeat Pap tests, HPV testing, or imaging studies depending on prior results.
Monitoring aims to detect recurrence or new cellular changes at an early stage. Regular evaluations help track cervical health over time and guide any further intervention if needed.
At The Women’s Center, we follow a structured approach to cervical health that begins with screening and continues through diagnosis and long-term follow-up. We carefully review Pap and HPV results, arrange timely colposcopy and biopsy when needed, and guide care based on clear clinical findings. When advanced treatment is required, we coordinate every step, including procedures such as hysterectomy for cervical cancer when appropriate.
If you have abnormal results or concerns, we invite you to contact us so we can review your situation and guide you with care and clarity.



Breast tissue contains a complex network of ducts, lobules, and connective structures, which explains why...
Read More
Abnormal Pap test results often begin the medical journey that answers the question of how...
Read More
Hormonal shifts after stopping contraception happen faster than many expect, yet timing still matters when...
Read More